Sponsored Content
Telemedicine opens the door to addiction recovery
Justin Schumacher started Independence Day with his usual routine: wake up at 3 or 4 a.m., walk downstairs and start drinking.
It was July 4, 2017 and Justin was battling a severe alcohol addiction. What had started as a way to self-medicate for anxiety and depression had spiraled into complete alcohol dependency. He knew he had a serious problem, but quitting felt physically impossible. An attempt to stop drinking had left him with a bloated stomach, yellowed eyes and overwhelming withdrawal symptoms.
There was also guilt. Instead of telling his wife, Justin put on his usual charming face and kept the problem hidden. The sickness every morning? Just stomach issues. And the yellow eyes? It must be old contacts, or maybe hay fever and wildfire smoke.
“It’s easily explainable when you’re charming and when your partner wants to believe that there’s nothing worse going on,” Justin said.

Justin Schumacher holds a cup labeled “The Friday the 13th Fun Fund.” To help take their minds off the uncertainty while Justin was hospitalized, Justin and his wife played a game where anyone who talked about the future had to put money in the cup. (Photo from Michael Fox)
But that morning, Justin’s charm ran out. His wife came downstairs to let him know she was leaving for work and opened the basement door to find him mid-drink. It was 5:30 in the morning. Justin compared it to a scene from the board game Clue, but instead of Colonel Mustard in the kitchen with the rope, it was Justin in the basement with a shot glass to his mouth.
Justin said his wife told him she had to leave for work but that they would talk about it later. She hoped he was okay. His first thought was that this must mean they were getting divorced.
That was the last day Justin drank. The expression on his wife’s face, which he can still picture today, is what made him stop, he said. It wasn’t disappointment or anger — it was a look of genuine concern; it was a look that said, “I love this person and I want them to be okay,” Justin said.
He now works as a peer coach with Boulder Care, a telehealth opioid and alcohol addiction recovery program based out of Portland. His work mainly involves building relationships with patients who are going through what he went through.
“It’s like the football player that comes home and coaches for the high school team,” Justin said. “You’re like, I was out in the world and I did it, now I’ve come back to teach others.”
Overcoming stigma
Justin was one of roughly 20 million Americans who suffer from substance use disorder. It’s a condition characterized by addiction to drugs or alcohol that often overlaps with other mental health disorders. For many, the combined stress and isolation of the pandemic has worsened the problem.
“I think you’d be hard pressed to find somebody who did not know somebody within their family or circle of friends that has struggled with substance use disorder,” said Susanne Quistgaard, medical director at Premera Blue Cross, which offers Boulder Care’s services with several of its medical plans.
Nobody chooses addiction, Quistgaard said. Substance use disorder is a disease that some people are more genetically predisposed to than others. It’s impossible for someone who isn’t prone to addiction to fully understand how powerful and all-consuming it can be.
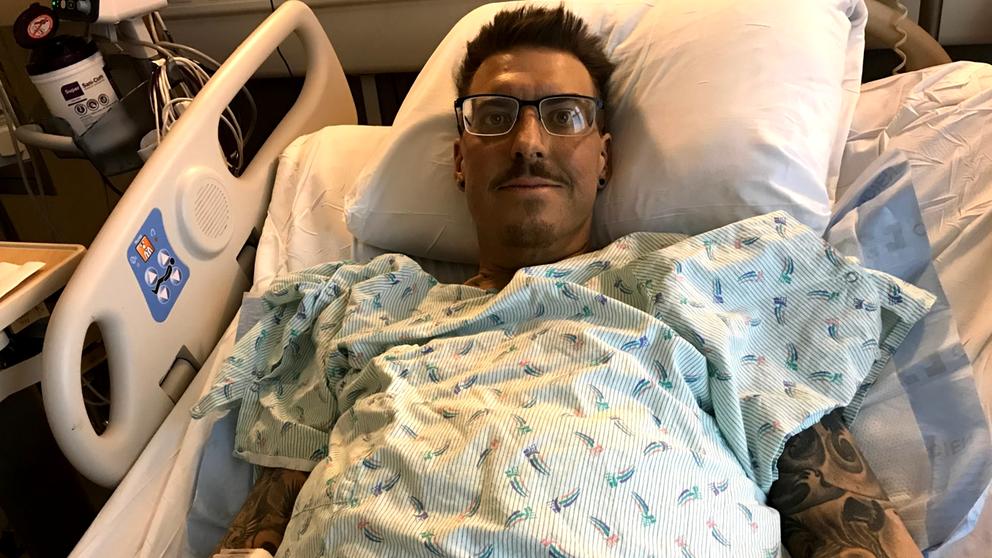
In July 2017, Justin Schumacher was hospitalized with severe liver and kidney failure. After being given emergency dialysis, doctors told him he might not live past September.
Negative perceptions of addiction persist. Of the 20 million Americans with substance use disorder, only 10% ever receive care. Quistgaard attributes the low number to ongoing shame and stigma.
As a peer coach with Boulder Care, Justin works with patients to help them develop goals and stay motivated through their recovery. He’s able to connect with them remotely through an app developed by Boulder Care.
Stephanie Strong, who founded Boulder Care in 2017, said peer coaches like Justin draw on their lived experience to connect with patients using language that is accessible, overcoming the stigma patients may have experienced.
Peer coaches like Justin are just one part of Boulder Care’s three-pronged approach to recovery. Patients are also paired with a clinician who can prescribe medications, ensure they’re getting the right dose and potentially help link them to other specialty or primary care. Care advocates work with patients to eliminate barriers that could be impeding their recovery. That could mean helping resolve pharmacy issues or working out concerns about insurance.
At Boulder Care, addiction is treated as a chronic condition, not something that can be solved in a couple of months. The goals that peer coaches help patients develop often involve quitting or reducing substance use, but they can also be things like finding stable housing or finishing college. At traditional residential or inpatient treatment centers, patients often leave after 30 or 90 days with no medication or support, which can make relapse more likely. Strong said Boulder Care has an 80% retention rate after 12 months, which is more than double the industry standard for outpatient care.
Boulder Care also practices a non-punitive approach to drug use. Many treatment centers regularly drug test patients and will kick them out if they’re caught using. At Boulder Care, patients are given encouragement and support during every step of the journey, even if they return to using.
Instead of drawing a hard line in the sand with a zero-tolerance policy, patients are able to make incremental changes towards healthier living. The concept behind Boulder’s non-punitive approach is “harm reduction,” that treatment should first and foremost limit the physical and emotional damage experienced by the person in recovery.
“The Boulder philosophy really is based in this evidence-based harm reduction and meeting people where they are,” Strong said.
Boulder Care’s philosophy also centers on giving patients a space to talk about what they’re going through. Strong said patients appreciate the opportunity to take an active role in their own recovery.
“You have to allow for people to talk about how they feel. And when we tell them not to do that, things fester inside of us,” Justin said.
Justin said listening is an important part of his work as a peer coach. Every time he meets with a patient, he’ll talk with them about what’s going on in their life, what goals they’re working towards, how they’re feeling about it. Sometimes a check-in is as simple as hanging out and saying hi, but mostly it’s about giving patients a space to talk about what's going on without judgement.
‘Team live’
Justin knows first-hand how important it is to be heard. Several days after the Fourth of July, Justin was hospitalized with liver and kidney failure. His legs and stomach continued to swell, and his eyes were an alarming shade of yellow. He remembers being surrounded with doctors peppering him with questions and accusations about his drinking:
“When did you take your last drink?”
“You’re going to kill yourself.”
“Thank God you didn’t drink another drink; you would have died.”
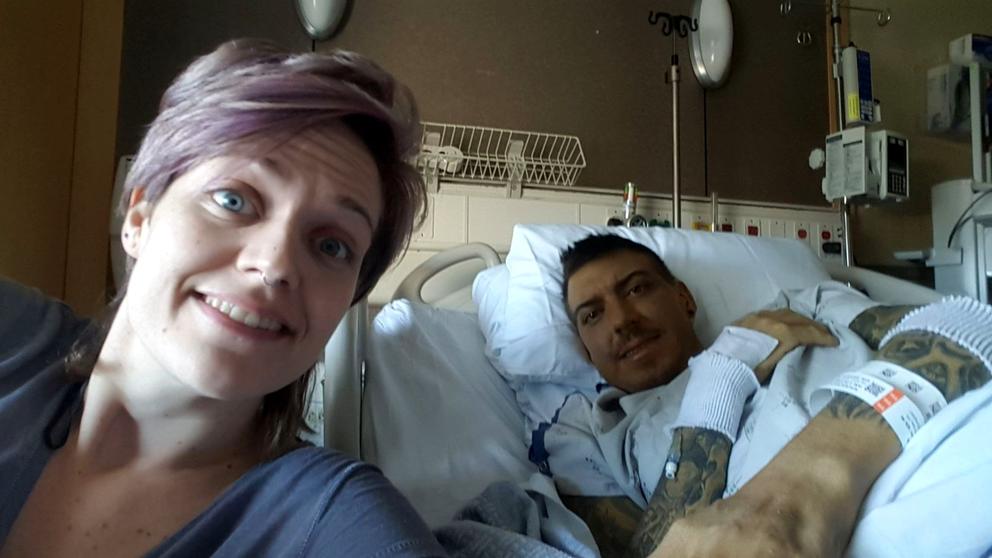
Justin Schumacher and his wife at a hospital in Oregon. Throughout his recovery, Justin said his wife’s honesty and support was essential. (Photo provided by Justin Schumacher)
Justin was given emergency dialysis. When he woke up, doctors told him there wasn’t much they could do and that he probably had until September. The hospital sent Justin home and he started doing dialysis three times a week. His health continued to deteriorate. He was hospitalized again, this time with a fever that came even closer to killing him. Around October, Justin went to a different hospital where he registered as a candidate for a liver and kidney transplant.
“That’s where the fun began,” Justin laughed.
The hospital told Justin and his family that the board had denied his request for a transplant. Because demand for livers and kidneys is higher than supply, many of the nation's transplant centers have informal policies that prevent people with alcohol-related liver damage from getting on the transplant list unless they can demonstrate six months of sobriety.
The next day (Friday the 13th, a date he remembers vividly) Justin asked the doctors what the appeal process was. They told him there wasn’t one; the hospital had made their decision. The doctors told him he probably wouldn’t make it through the weekend and asked if he would rather die in the hospital or at home.
Justin weighed the options in his head and identified two different paths: Team Live and Team Die. Justin thought about unplugging the dialysis machine and buying a ticket to Hawaii with his wife so he could jump in the ocean and get eaten by a shark. It wouldn’t be pretty, but it sounded a lot cooler than dying after spending hours hooked up to a machine. But Team Die also meant finality — if he chose Team Live, there was still a chance.
Justin chose Team Live.
“I didn’t know what was going to happen next, but what I did know was that I needed to be in the moment,” Justin said.
Justin's parents, his wife, his wife’s parents and his wife’s best friend were all in the hospital with him. Together, they started playing a game where anyone who talked about the future had to put money into a cup they had labeled “The Friday the 13th Fun Fund.”
“It was about staying present, because we knew there wasn’t going to be tomorrow promised,” Justin said.
Justin woke up the next day, and then the next day after that. On Oct. 15, Justin said one of the liver doctors saw something different and got in touch with a doctor at another hospital in Seattle who did transplants.
“I was treated completely different; I was treated like a person and not an alcoholic,” Justin said.
Justin was added to the transplant list on Oct. 22. Six days later, he had a new kidney and liver.
When people asked what was going on, Justin said his wife didn’t try to hide the truth. She told them bluntly that Justin was in the hospital because he was an alcoholic, and that he drank because he had anxiety and depression.
Justin said he was inspired by his wife’s honesty and support. When he left the hospital in 2018, he started taking classes to become a drug and alcohol counselor and peer coach. His first job was with the addiction team at the same hospital where he had been denied a transplant. He later connected with Dr. Alyson Smith, the medical director of Boulder Care.
Justin said he was instantly drawn to Boulder Care’s model of kindness and support. As COVID began to sweep the country, Smith reached out to let Justin know that a peer coaching position had opened up. Justin applied right away.
“I want to work for a place that treats people like people and disease like disease,” Justin said. “And that’s how I found Boulder.”
Meeting people where they are

Boulder Care’s telehealth model breaks down access barriers and allows peer coaches like Justin Schumacher to connect with patients wherever they are. (Photo provided by Michael Fox)
In 2020, Boulder Care partnered with Premera Blue Cross, a leading health-care provider in the Pacific Northwest. Strong said the partnership has helped them expand Boulder Care’s reach and provide in-network coverage to an even broader range of patients — from technology executives in Seattle to people in rural Alaska who live two flights away from the nearest treatment center.
“Premera has more options to connect our patients with care now,” Quistgaard said. “So now no matter where patients live, we can connect them with Boulder Care and we know they’ll be getting high quality, evidence-based care for their substance use disorder.”
Quistgaard said the partnership helps break down the barriers of privacy and stigma that have challenged addiction recovery efforts in the past. Patients no longer have to worry about running into someone they know, and can fit their treatment around their own work or childcare schedules.
Before starting Boulder Care, Strong worked in healthcare investing and consulting. The work sometimes took her to addiction treatment centers in rural Massachusetts, where she said people sometimes saw people commuting by skateboard in the middle of winter just to get to the nearest treatment facility. Boulder Care’s virtual care model allows peer coaches like Justin to connect with patients anywhere. Sometimes that means churches, hospitals, McDonald’s parking lots or in homes with children sleeping.
Prior to the pandemic, patients were required to have at least one in-person meeting with a physician before they could be prescribed medications, like buprenorphine, which is used to treat opioid withdrawal. The law was suspended during the onset of the pandemic, making it easier for patients in rural areas with few doctors to access the medications.
“At Premera, we feel very strongly about doing the right thing. And clearly doing the right thing includes offering increased access to our customers with substance use disorder,” Quistgaard said.
While Justin hasn’t had a drink since 2017, he said the disease never went away. The support he receives and the work he does to help others has helped keep him motivated.
“It would be easy to pick up a drink. It would be easy to pick up a drug. I don't, because I'm surrounded by people that embrace me for all of the things that are going on inside," Justin said.
People struggling with substance use disorder can visit Boulder Care’s website to look at options or chat with a Boulder Care agent. Staff are also available for guidance over the phone at 503-447-8712.

