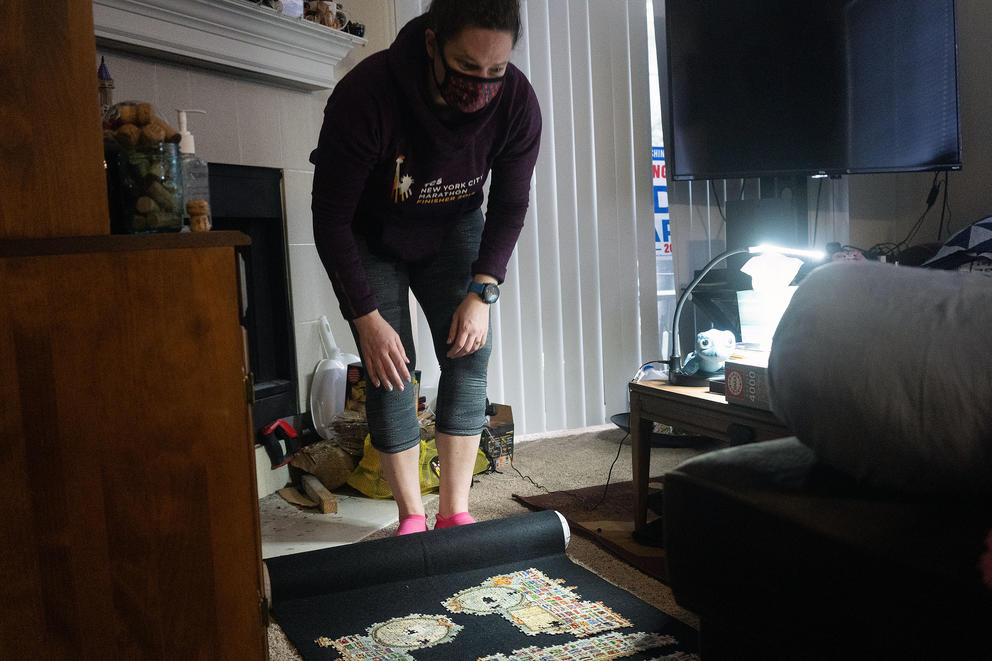In conversation, she said, she sometimes struggles to find the right words and loses her train of thought. Computer games are too complicated for her to follow, and she remains on leave from her job as a nurse case manager for Premera Blue Cross because she believes she can’t bring her A game to patients.
Puzzles bring some solace — “it’s a way to think about one thing at a time and work my way through a process” — but Hayes said she feels lonely because very few understand firsthand what she is going through, and it’s difficult to describe. Hayes is not even sure where her brain fog begins and her physical symptoms end, and she has no idea how long it will last.
Doctors don’t know enough about COVID’s little-understood effects on the brain to advise patients like Hayes. But the long-lasting brain damage similar to what Hayes suffers has scared University of Washington researcher Dr. William Banks enough to try and advance the cause.
Robin Elizabeth Hayes spends much of her time at home in Issaquah living with COVID-19 long hauler symptoms since her diagnosis in January. "Doing puzzles helps keep my brain active and battles the constant brain fog that I'm experiencing," said Hayes, who has recently undertaken a 4,000-piece puzzle during her recovery. (Matt M. McKnight/Crosscut)
“My personal fear is not so much with death, but with incapacity,” he said.
Many symptomatic COVID-19 patients struggle with breathing, coughing, fever and fatigue. But even after recovery, a growing subset of patients has been struck by so-called “long COVID,” wherein adverse symptoms linger for six months or more. The most common symptom is referred to as “brain fog.” Symptoms vary, but they include memory loss, confusion, trouble finding words, difficulty in concentration. memory loss and a general feeling of being overwhelmed.
“COVID in the brain is going to be a huge issue, and we’ve got to get a handle on this,” said Banks, a professor of medicine at the University of Washington School of Medicine.
So how does a respiratory disease lead to neurological troubles in the brain?
Last December, Banks and his roughly 15-person research team published a study in Nature Neuroscience that showed the possible path this respiratory virus travels to cause fuzziness in the brain. Follow-up studies are needed to verify their hypothesis, but the gist is that the SARS-CoV-2 virus — which causes COVID-19 — can enter the brain by using the spikelike S1 proteins that cover it to pierce the blood-brain barrier that protects it.
Dr. William Banks works at the Veterans Administration of Puget Sound and is leading research for the University of Washington on how COVID-19 can cause brain fog and long-term issues for the brain after you get it. Photographed at his home in Seattle's Beacon Hill neighborhood on April 5, 2021. (Matt M. McKnight/Crosscut)
The blood-brain barrier is a semipermeable membrane filter that allows some microscopic nutrients (like glucose, water and amino acids) to pass from the bloodstream into the fluid surrounding the central nervous system. That process affects the firing of neurons, which carries the brain’s messages throughout the body.
In their experiment, Banks and his team injected radioactive S1 proteins from the SARS-CoV-2 virus into up to 100 mice in the laboratory. (For safety reasons, the actual virus could not be used.) The mice were then euthanized, and their brains were examined for the presence of the radioactive protein. “It turns out that the S1 does get in,” Banks said.
Once the S1 protein uses its armlike feature to hook into the blood-brain barrier and seep through, it can possibly cause inflammation in the brain. That inflammation might be the cause of this mysterious brain fog.
Robin Elizabeth Hayes, who was diagnosed with COVID-19 in January, has since been suffering from long hauler symptoms that include debilitating brain fog and pulmonary issues that have sidelined her from her work and training as an athlete. "My doctor has told me not to spend more than five minutes per day doing any exercise," said Hayes, lamenting her inability to train and having to endure general exhaustion daily. "I'm working with my pulmonologist and we're trying to figure out how to get back the lung function I once had." Photographed at Lakemont Park in Issaquah, on April 8, 2021. (Matt M. McKnight/Crosscut)
Since COVID-19 has been studied for barely more than a year, the research that exists on its effects on the brain is limited — including how many COVID patients suffer from brain fog. But scientists guess that long COVID could eventually plague between one in 10 and one in three Americans who contract the disease.
“It’s a brain disease as well as a respiratory disease, and needs more research,” Banks said.
Banks’ lab switched to COVID-related research a little more than a year ago, when the scope of the disease’s impact became apparent. Before the pandemic, the lab for many yeas studied the blood-brain barrier’s role in Alzheimer's disease, obesity, diabetes and HIV.
Meanwhile, a Johns Hopkins University study published Feb. 12 found another clue to how SARS-CoV-2 affects brains. In autopsies of 15 COVID-19 victims, that research found megakaryocytes in the capillary blood vessels of the brains of a third of those fatalities. Megakaryocytes are large bone marrow cells responsible for the production of the platelets, which enable blood clotting, and they are not usually found in the brain. Megakaryocytes have been found in many of the myriad organs coronavirus affects, like the lungs or kidneys.
Banks said one major factor in future research is to confirm that what happens in a mouse’s brain can be extrapolated to what happens in a human’s brain. Banks’ lab also hopes to get a hold of an artificial, noninfectious virus to duplicate the previous work done with just the S1 protein. This could help fulfill Banks’ ultimate goal: to discover precisely how COVID-19 causes brain fog.
“Next question is why,” he said.