Sponsored Content
A creative approach to rural, community health care
In movies, books and folklore, Alaska is often portrayed as a land of severe weather and punishing living conditions — and for good reason. Average wintertime temperatures in Anchorage, the state’s largest city, barely reach double digits, and the wind chill can plunge the mercury well below zero for weeks on end.
Life gets even tougher in areas like Alaska’s Yukon-Kuskokwim Delta, a region the size of Oregon with a population of just over 30,000 people. Located 400 miles northwest of Anchorage near where the Yukon and Kuskokwim rivers empty into the Bering Sea, the region experiences weather even more extreme, and life’s necessities can be hard to come by.
The Y-K Delta is dotted with 41 rural communities, most ranging in size from 25 to around 1,000 people. The majority of the residents — around 85 percent — are Yup’ik- speaking Alaska Natives. The largest Delta village is the city of Bethel, with around 6,400 residents. None of villages are connected by roads; residents turn to airplanes, boats, and, in the winter, snowmobiles to get around.
The delta’s only full-service health care center is in Bethel, and most of those living in the villages have difficulty reaching it. So the Y-K Delta’s residents have come to rely on their neighbors to meet their health care needs.

Training to care for their neighbors
The Community Health Aide Program, or CHAP, was founded in the 1960s as a way for far-flung villagers to access basic medical services without traveling far. To become a community health aide, members from the delta’s villages come to the Yukon Kuskokwim Health Corporation in Bethel for an intensive program that includes classroom instruction, hands-on training and in-clinic practice.
The training program gives aides the skills to provide a number of services, including eye exams, diagnosing ear infections, setting broken bones, and responding to emergencies. Other programs train aides to provide dental and behavioral health care. Once certified, the aides head back to their villages to start seeing patients, assisted by an interactive manual on their iPad and close communication with physicians back in Bethel.
The community health aide program recently caught the attention of some in the lower 48. Health care providers, tribal agencies and underserved populations in Washington, Oregon and elsewhere see the value of CHAP’s community-based, culturally sensitive approach and are reaching out to coordinators so they can implement similar programs.
Community ties run deep
Katherine Evon spent three years as a community health aide in her home village of Akiachak, 18 miles up the Kuskokwim River from Bethel. Like many villagers who train to serve as health aides, she was already familiar with the program. She grew up watching her mother, herself a health aide, treat others in their small village. “The level of care she gave inspired me to do something like that as well,” says Evon, who now works as a CHAP field coordinator.
In the villages, family and community ties run deep, and health aides wear their CHAP certification with pride.
“You leave the village knowing you are going to come back and provide for your people,” Evon says.
Phillicia Charlie came from her home village of Kwigillingok, 70 miles from Bethel, for community health aide training. She worked in the hospital in Bethel as a certified nursing assistant after she graduated from high school, but felt the pull of her roots. “I wanted to go back home,” she says.
Training as a health aide will allow her to provide care for others in the place she most wants to be.
That cultural connection between villagers and their resident caregivers is one of the main tenants of the community health aide program. Many share the Yup’ik language, and resident caregivers understand lifestyles and habits that can help shed light on ailments or issues patients are experiencing. This common thread goes a long way towards the quality of care villagers receive.
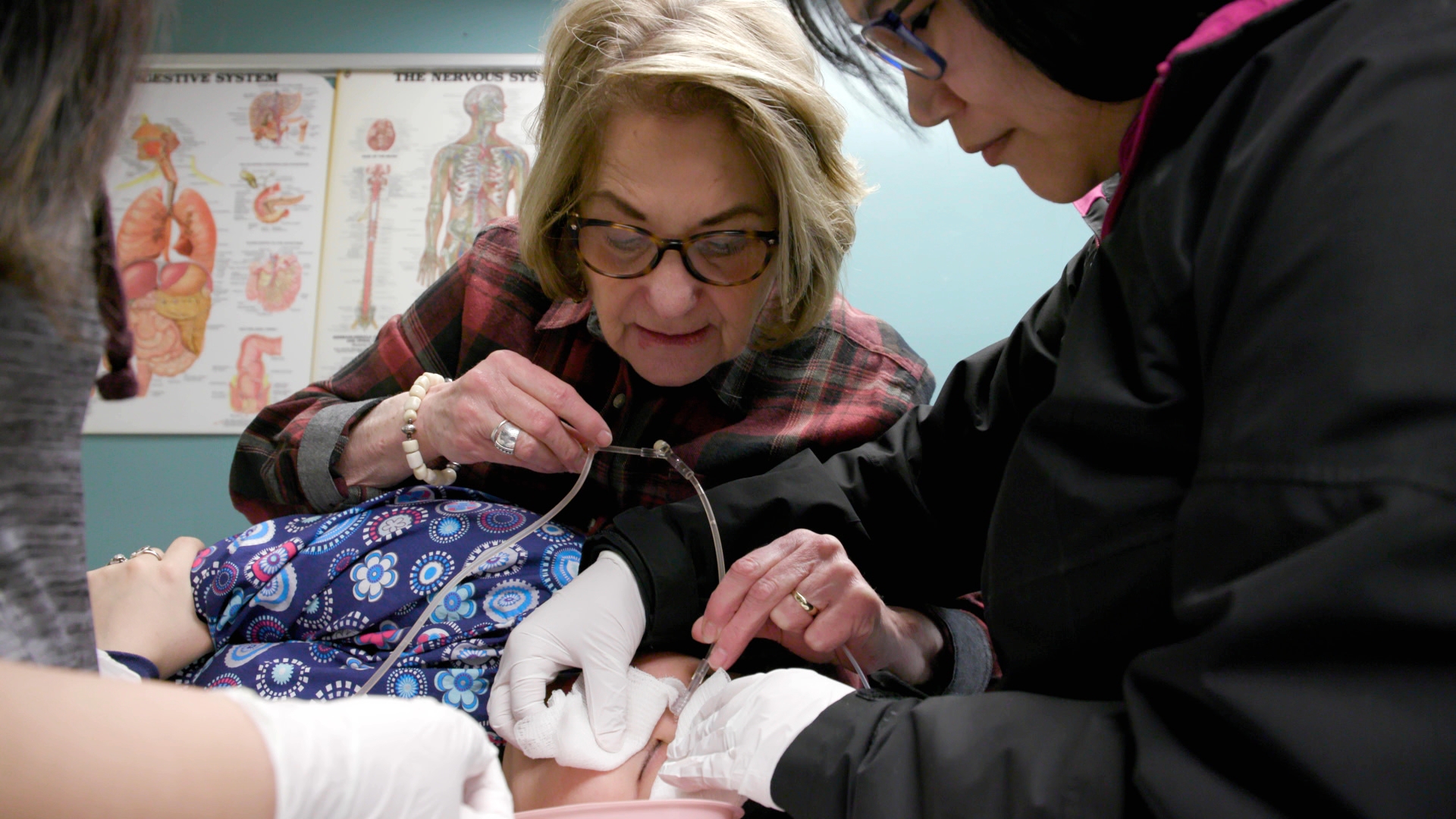
“Health aides are often referred to as the heart of the Y-K Delta,” says Rahnia Boyer, vice president of village health with the Yukon-Kuskokwim Health Corporation, one of four organizations in Alaska to offer CHAP training under a contract with the federal Indian Health Service. YKHC oversees the care of 30,000 people and manages 41 village clinics, most staffed only by a health aide and an office assistant. “Not only do they understand the area, but they are from the area.”
Care across the spectrum
Just as important as the CHAP’s cultural connections is the quality of care the health aides provide. Residents tell stories of the days before health aides, when villagers would wait weeks — or longer — to see visiting doctors. The infant mortality rate was high and the absence of much needed medications meant tuberculosis was rampant. Villagers would forgo preventive care rather than spend hours or days traveling — or paying hundreds of dollars for round-trip airfare — to visit a health care provider in Bethel.
With trained health aides living within minutes of their patients, “we prevent a lot of that from happening,” says Chet Ford, a nurse practitioner with YKHC who oversees an advanced care program for the Y-K Delta’s villages. “We take the care to them so they don’t have to come to us.”
The level of training the aides receive is high, allowing them to perform routine and emergency medical care. A day may include a house call for a sore throat, treating a patient with a concussion and setting a broken bone. They’re often the first on-scene when there’s a hunting accident or heart attack. To prepare for such a wide range of care, health aides complete four sessions of community health aide training, each lasting three to four weeks. Between sessions, trainees work in clinics completing a skills list and practicum. After successfully completing the four-session training curriculum and a clinical skills preceptorship and examination, the trainee qualifies as a community health aide.
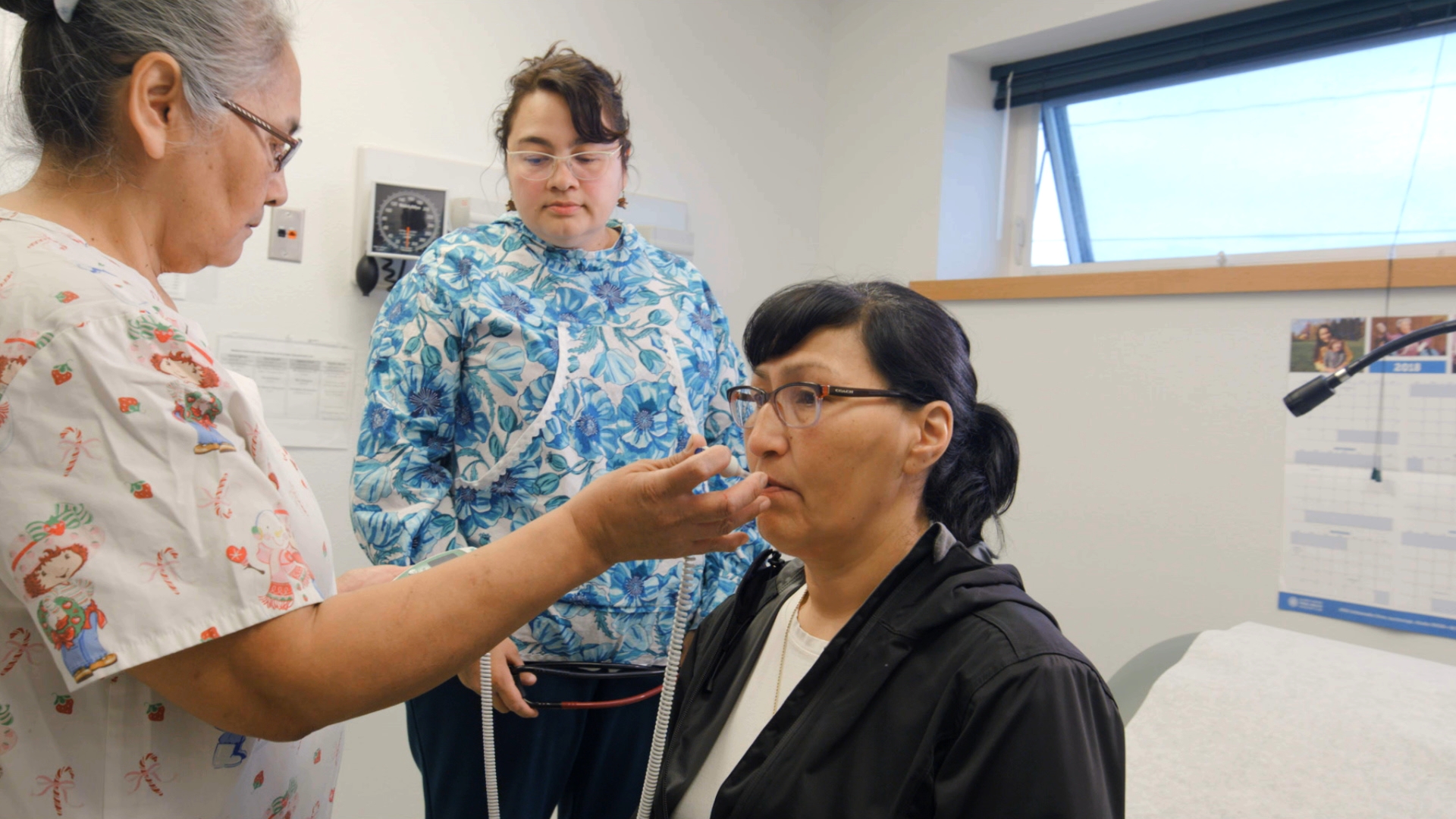
Sharing the knowledge
The success of the community health aide training program has not gone unnoticed by organizations and agencies outside of Alaska. Representatives from community health centers in Washington, Oregon, Idaho, Montana, Arizona – and even Liberia – have reached out to state agencies for information.
The program is a good fit for populations that are not only geographically isolated from health care hubs, but perhaps culturally isolated as well, says Bob Onders, a medical director for the Alaska Native Tribal Health Consortium, an agency supporting Alaska’s community health aide training program.
“The traditional health care education model overvalues technical competency and undervalues the community and cultural aspects of healthcare,” says Onders, himself a physician. Veterans, the homeless, Native American tribes and other populations that may be socially separated from mainstream society can be served well by health aide programs, he says. “My feeling is that there are just as many isolated communities in Seattle or Los Angeles as there are in Alaska.”
While the CHAP is currently only approved for practice in Alaska, Indian Health Service is considering nationalizing it. In 2018, IHS formed a CHAP advisory group to expand the program to the lower 48 states.
Investing in rural care
Premera Blue Cross Blue Shield of Alaska recently made a $5.7 million investment to support access to rural health care in Alaska. The health plan provider has established the Rural Health Care Fund, managed by the Rasmuson Foundation, that will be used to award a wide variety of grants addressing equity, availability and access to quality health care in rural areas. YKHC’s community health aide program is one of three programs in Alaska that has received a grant of up to $100,000 to support small capital improvements, equipment purchases or other needs critical to expanding the CHAP’s reach.
The outreach underscores Premera’s interest in improving the health of people living in underserved areas. According to a 2017 study by the National Rural Health Association, people living in rural areas suffer worse health outcomes than their urban counterparts. They are sicker, poorer and older, and are more likely to experience higher rates of premature death, disability and chronic disease. In Alaska, more than 200,000 people, or about 32 percent of the state’s population, live in rural communities.
“It is critical to invest in effective, long-term solutions to close the growing gap between urban and rural health care access,” says Jeff Roe, president and CEO of Premera Blue Cross.
‘These are their people’
Before Marsha Smith took a position as a CHAP training instructor, she served as a community health aide in her home village of Scammon Bay. The job was rewarding and fulfilling, but a series of emergency calls that kept the village’s health aide response team camped out at the clinic for three consecutive nights proved to be so stressful that Smith took a leave of absence. But after a month she returned.
“I couldn’t stay away,” Smith says. “You know everyone in the village. When you hear someone calling and needing help, you just want to be there.”
Smith’s story doesn’t surprise YKHC’s Boyer.
“It’s very personal care,” Boyer says. “These are their people they’re taking care of.”

