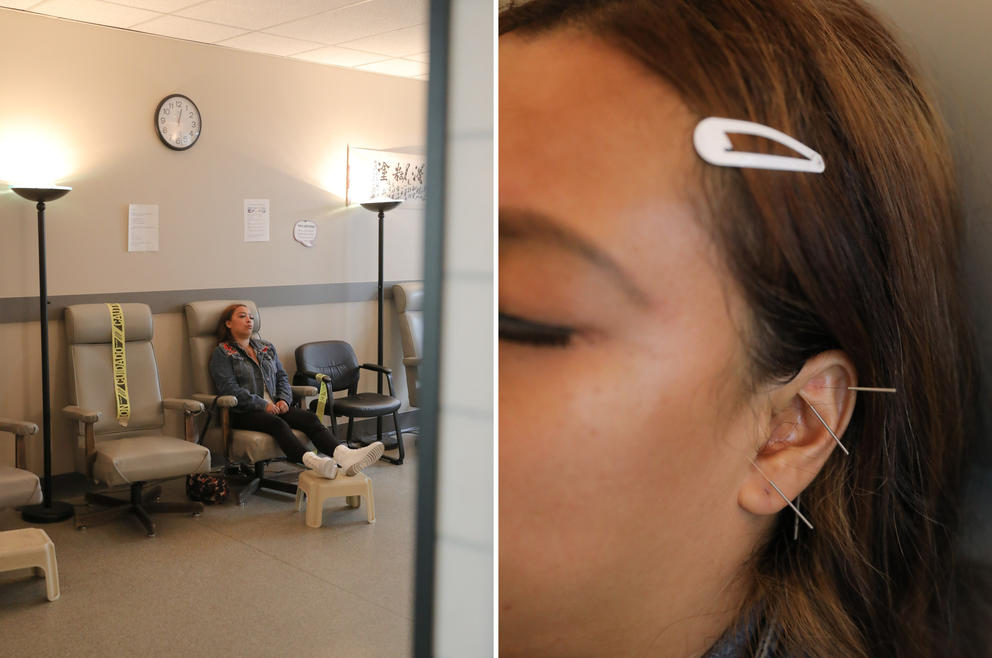
Sunny comes to the clinic six days a week to get her daily dose of the highly regulated opioid-treatment drug, though, she said, she’ll soon complete an orientation that will reduce the chore to three days a week. She’s struggled with addiction on and off throughout her life, and relapsed after fleeing domestic violence and ending up homeless.
“It’s so hopeless when you’re homeless,” said Sunny, who provided only her first name to Crosscut. “It doesn’t matter why you become homeless. Once you are, everybody treats you differently.”
Sunny has since moved off the street and is trying to work through the red tape to get her own affordable-housing unit. She said she knows medication is only part of the solution for her addiction, and that there are traumatic things from her past that she needs to deal with someday. “A lot of treatment centers treat the symptom, but don’t get at the root of why you’re using in the first place. You need counseling and therapy.”
She is one of countless people caught up in Seattle’s worsening addiction crisis — a crisis shared by the region, state and country. In 2022, 1,001 people in King County died of drug or alcohol overdose, according to data from King County’s Public Health Department. Of those deaths, 712 were attributed to fentanyl. Now, a little more than halfway through 2023, the county has already recorded 761 overdose deaths, 617 attributed to opioids.
Elected officials in Seattle are currently debating how to best deal with the crisis, or at least with its public face. City Councilmembers Sara Nelson and Alex Pedersen introduced legislation in June that would have put on Seattle’s books a new state drug law making possession and public use a gross misdemeanor. Doing so would have given the Seattle City Attorney Office authority to prosecute drug possession and use cases for the first time, rather than leaving them to the King County Prosecutor.
The bill narrowly failed. Supporters said arrests and jail are an important path to move people toward treatment. Detractors said jail is the wrong way to treat a public health issue. Though they disagreed on the approach, both sides said their goal was to get people with substance-use disorders into treatment.
But what exactly do we mean by treatment? What does it look like to try to access services in the Seattle area? Is jail actually an access point for help? What needs to change to ensure the treatment system meets the scale of the fentanyl crisis?
Crosscut spoke to drug treatment service providers, advocates, researchers and public health officials to help answer those questions.
What is drug treatment?
The drug treatment landscape in the Seattle area is vast, ranging from low-barrier harm-reduction work to lengthy residential inpatient treatment centers. The core of substance-use disorder treatment falls into three categories: medication-assisted treatment, outpatient treatment and inpatient treatment.
People find their way to treatment in a variety of ways: upon referral by an outreach worker, at the insistence of family or friends, through drug court or another diversion program, by emergency room referral or, as is often the case, of their own accord.
Harm-reduction work like needle exchanges, distribution of the overdose-prevention medication naloxone, mobile meal distribution and medical outreach are not considered forms of treatment per se, but they are an important frontline piece of the puzzle. They help keep people alive until they’re ready to seek more formal treatment options.
Experts say peer counseling and group talk sessions such as those provided by Recovery Café and Peer Seattle are another important, lower-barrier entry point to recovery. For someone experiencing substance-use disorder, a peer who’s been through similar traumas is often a more trustworthy source of help than more institutional options. Those providers also typically help refer clients to other more formal treatment methods.
There are also many Narcotics Anonymous and Alcoholics Anonymous group meetings hosted throughout the Seattle-area that use the 12-step approach to recovery.
Medication-assisted treatment (MAT) for opioid substance-use disorders uses doses of synthetic opiates such as methadone and buprenorphine to stave off cravings and withdrawal symptoms. The goal is to stabilize people before they enter counseling to address the root causes of their substance-use disorder and provide tools to deal with addiction.
MAT tends to be relatively low-barrier, with most providers offering walk-up, same-day service without a referral. But MAT access is not without challenges. Clients must make it to the provider during business hours. Transportation can be a challenge for those relying on public transit. People must go through a lengthy intake process to start. Because distribution of the medication is highly regulated, clients must come six days a week to get their doses for at least the first six months — a logistical challenge for anyone, let alone someone in the throes of addiction.
On top of that, federal methadone regulations allow a maximum first dose of 30 mg, which doesn’t do much to ease withdrawal symptoms from heroin and does even less for a fentanyl user.
“One of the difficult parts for us is we’re asking people to take medication that will help them eventually, but [which] in the moment of most need is not going to do much to help,” said Sean Soth, Evergreen Treatment Services director of health innovation. “Some of the archaic rules are making it difficult by not reducing withdrawal symptoms or impacting craving in any major way with that little of a dose.”
MAT is just one step of the treatment process. Some MAT providers, such as Evergreen, also provide other services to aid with recovery: counseling, group talk sessions, even acupuncture to alleviate withdrawal symptoms and pain.
The next levels of drug treatment are outpatient, and intensive outpatient treatment followed by inpatient treatment. Outpatient treatment involves weekly therapy sessions with licensed professionals who provide one-on-one counseling. Treatment centers often offer relapse education and continuing care plans for clients to draw on once the treatment ends.
Intensive outpatient treatment entails longer therapy sessions three to five days a week, and often includes group therapy in addition to one-on-one sessions. Many outpatient providers require abstinence from substances to participate.
Inpatient treatment is a residential service in which clients stay onsite for a set period to detox. They also go through therapy and counseling.
Though the counseling and therapy provided through outpatient and inpatient treatment is seen by many as key to sustained recovery, both come with challenging barriers to access. Any client seeking treatment must first make an appointment for an in-depth assessment, a process that can take anywhere from 90 minutes to three hours.
That alone can be a challenge for someone “in various types of withdrawal or crises that make it difficult to sit through a two- to three-hour assessment or keep appointments,” said Mandy Owens, a clinical psychologist and professor at the University of Washington’s Addictions, Drug & Alcohol Institute.
On top of that, some experts say the assessment, which requires going over usage history, family history, past incarceration and other potentially traumatic subjects, can be damaging to someone in the vulnerable position of withdrawal.
“When somebody is using, it is not a good time to trigger their painful past,” said Karen Lizzy, a licensed mental health counselor and substance-use disorder professional with the Cowlitz Indian Tribe. Lizzy is a citizen of the Bay Mills Indian Community, a band of Ojibwe in Michigan.
“There’s buzz about trauma-informed care. But I say shame-informed care,” Lizzy said. “How are you not going to both trigger trauma and avoid hitting shame? It’s everywhere in our systems.”
Once someone makes it through the assessment process, there is often a waitlist to get into outpatient programs and almost always a waitlist to get into inpatient treatment, due in part to the industry’s high turnover and challenges retaining staff. It’s a problem found in nearly all corners of the human-services sector, where low pay and increasingly difficult work has led to widespread burnout.
The high turnover can also harm clients’ progress. Trust is a key element of recovery, but it’s hard to build with clients. “You have a person who’s developed some rapport with a staff member, and it’s extremely jarring for them to have a new staff person come in and take over,” said E.V. Velez, a recovery support coordinator with Snohomish Superior Court who’s worked in both inpatient and outpatient settings.
Inpatient treatment also suffers from a dearth of physical space. Because of budget cuts and other factors, King County has lost at least half its residential treatment beds since the 1990s, leaving about 260 remaining today.
These delays can result in missing somebody’s “window of willingness,” a term for the often-brief moments a person suffering from addiction decides they want to seek help.
“The window of willingness can close up and they’re using again. We lose people,” said Heather Venegas, King County Recovery Coalition director.
Does jail provide drug treatment?
The short answer is yes, people can access treatment in jail in King County. Those with substance-use disorders can begin or continue medication-assisted treatment for withdrawal symptoms while incarcerated.
Service providers such as Pioneer Human Services also contract with King County to provide treatments such as group therapy and counseling in jail. They also conduct assessments and make plans to help people access other services once they leave jail.
Service providers broadly agree that jail can help put people on a path to recovery — but also that it’s not an ideal setting.
“Can it help people recover? Of course,” said Owens. “I have heard many stories about how incarceration gave someone a break in substance use and allowed them to access services, and it was a turning point in their recovery journey.”
But Owens and many other experts Crosscut spoke to also said jail is a traumatic place that can exacerbate the root issues of someone’s substance-use disorder, and that the often-short stays don’t provide time to really make a difference.
Joe Miller, Pioneer Human Services’ director of transition services, is proud of the work the organization does with people experiencing substance-use disorder in jail, but acknowledges it can be a difficult environment for treatment.
“The setting can be quite challenging at times just from the human element,” said Miller. “Because they’re in jail, they don’t have the opportunity to go and create a broader network of positive influence. They have to have the ability to create it amongst themselves.”
“Carceral systems are created as systems of punishment,” said Brad Finegood, a strategic advisor for Public Health – Seattle King County who works on overdose prevention. “Punishment is not necessarily meant as a treatment option. We believe and know people heal in community. We want to provide as many options as possible to heal in community.”
How can the treatment system improve?
Everyone Crosscut spoke to for this article agreed that improving access to treatment by reducing wait times is a key step toward addressing the addiction crisis.
The forthcoming King County crisis care centers — funding for which was approved by voters in April — are meant to address some of the many access issues people currently face. The centers will be open 24/7 and allow drop-in assessments and referrals. They will also provide short-term beds where people can stay for up to 14 days before discharge or referral to other services.
The voter-approved property tax will pay for five centers around King County, including one specifically for youth. But, having been funded only this year, the centers are years from completion.
Another way to increase access is to bring treatment to people instead of requiring them to travel. Evergreen Treatment Services recently launched a mobile methadone clinic in Seattle. We Care Daily Clinics is another service provider operating a mobile opioid treatment clinic in Seattle that offers medication-assisted treatment as well as assessment and referrals.
Several providers and advocates say stigma around drug use and addiction is a huge challenge, both within the treatment system and in the public understanding of substance-use disorder.
“There’s still stigma around using, and an idea that you have a choice to do that,” said Lizzy of the Cowlitz Tribe health services. “Do I have any more or less of a choice that my brain says to kill myself by using [drugs] than if I said I was going to kill myself with a gun or knife? Why is that manipulative?”
“If treated, people recover, they live healthy lives,” said Finegood. “We need to continue to humanize the condition. We need to continue to work to allay stigma.”
UPDATE: This article was updated to include information about 12-step Narcotics Anonymous and Alcoholics Anonymous meetings as another available treatment option.